Provider data accuracy has moved from an operational concern to a regulatory and financial risk. Inaccurate provider directories lead to ghost providers, incorrect contact information, and outdated network status. These errors affect compliance under the No Surprises Act, expose health plans to financial liability, and hurt care delivery, member satisfaction, and patient outcomes.
For large national and regional health plans alike, provider data errors are not isolated mistakes. They reflect systemic weaknesses in provider directory management. This article outlines the most significant provider data challenges today, why traditional approaches fall short, and what structured validation looks like in practice. For a broader strategic framework, see our comprehensive guide to Provider Data Management here.
Why Provider Data Accuracy Has Become a Strategic Risk
Federal regulation has changed the stakes. With the signing of the REAL Health Providers Act, plans must verify network status every 90 days and update directories within two business days of receiving new information. If a member relies on incorrect directory information, the plan bears the financial risk. Read more about the REAL Act here.
This shift creates three executive-level implications:
- Compliance exposure tied directly to directory accuracy
- Financial liability for out-of-network claims caused by inaccurate listings
- Reputational damage when members cannot access listed providers
Inaccurate provider directories are no longer a back-office data hygiene issue. They are audit-visible operational risks.
The Biggest Provider Data Challenges in Healthcare Today
Ghost Providers and Ghost Locations
Ghost providers remain one of the most persistent issues. These include retired clinicians, relocated providers, or providers listed at locations where they no longer practice.
In network adequacy terms, this distorts members’ actual access to healthcare services. A directory may list 1,000 behavioral health providers in a county, but a material percentage may not be actively practicing there. This creates artificial network strength on paper while members experience access gaps.
Ghost locations create similar distortions. Plans may list providers across multiple addresses, even when only a subset are valid. Some plans see more than 40% of their provider addresses flagged as inaccurate upon first analysis.
Provider Directory Errors Across Core Attributes
Provider directory errors extend beyond addresses. Phone numbers, specialties, accepting-new-patient status, and hospital affiliations frequently diverge across systems.
A peer-reviewed JAMA study, conducted with the University of Colorado, found that:
- 81% of physicians had incorrect directory entries,
- 72% had inconsistent practice addresses across directories, and
- 32% showed inconsistent specialty information.
These discrepancies are not marginal. They indicate structural weakness in provider data management.
Fragmented Systems and Manual Verification
Large plans often operate across multiple systems: claims platforms, credentialing tools, provider relations databases, and public-facing directories. Updates do not propagate consistently.
Manual processes remain common. Call campaigns, provider attestations, and self-reported updates are resource-intensive. Industry-wide, manual verification costs exceed $2 billion annually. The result is a lag between data change and directory correction. During that lag, compliance risk accumulates.
Why Traditional Fixes Do Not Scale
Many organizations address provider directory errors through periodic clean-up projects. These efforts produce temporary improvements but do not solve underlying structural issues.
The limitations are predictable:
- Verification cycles tied to quarterly or annual audits rather than ongoing refreshes
- Sampling-based validation instead of comprehensive review
- Unscalable, manual reconciliation across disconnected systems
- Limited visibility into which attributes are most unreliable
This reactive model cannot meet the regulatory cadence. CMS requires directories to be updated within 30 days of information change, with additional requirements for verification frequency.

Continuous validation shifts the operating model from episodic correction with ongoing oversight.
A Structured Approach to Provider Directory Management
A structured approach to provider data accuracy includes four components:
- Cross-source validation
- Attribute-level scoring
- Regular refresh cadence
- System-level integration
HiLabs® MCheck® Provider Data Accuracy (PDA) applies a healthcare-specific LLM and VLM backend to analyze provider data across thousands of public and private sources. The system scores provider records based on reliability, relevance, and recency (the HiLabs R3 model).
Validation typically runs on a regular, customizable cadence. The objective is sustained directory accuracy rather than periodic correction. HiLabs has corrected over 100 million provider data errors for 10+ national and regional plans while maintaining 95%+ directory accuracy.
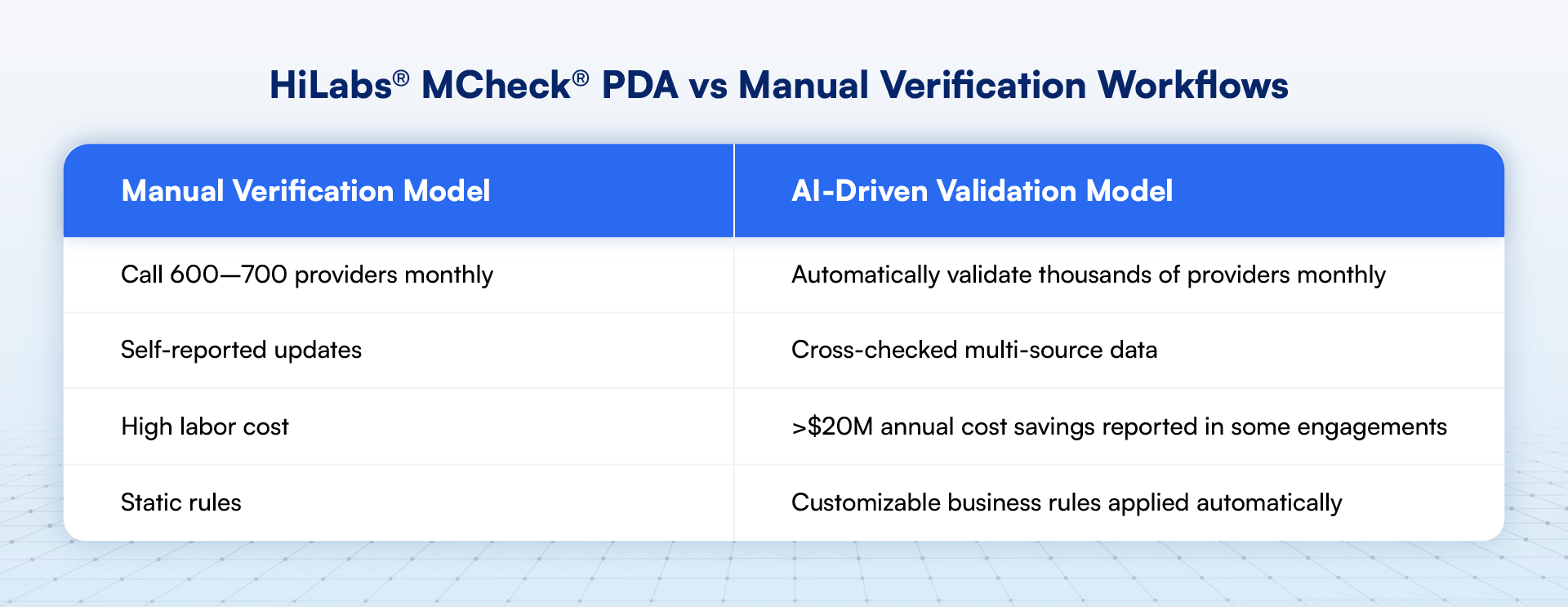
Customizable business rules allow plans to define validation criteria. For example, plans may restrict claims-based address validation to claims from the last three months. This ensures validation aligns with operational context.
Real-World Provider Data Impact
In one national plan engagement, HiLabs® processed over 2 million records across 26 markets over two years, with over 95% recommendation accuracy. These improvements affect more than directory appearance. They improve CMS audit performance, reduce member abrasion, and provide clearer visibility into actual network adequacy.
Why Provider Data Accuracy Matters in 2026
Regulatory enforcement has increased scrutiny on provider directory accuracy. Under the No Surprises Act framework, financial liability shifts to the plan when directory data is incorrect. Simultaneously, network adequacy requirements demand accurate representation of active providers in each geography. Without reliable provider data accuracy, network adequacy assessments are speculative.
For executive leaders in provider data management, network operations, and compliance, this is a governance issue. It requires defined workflows, traceable validation logic, and measurable performance.
Connecting Provider Data Accuracy to Broader Strategy
Provider data accuracy is one dimension of a larger provider data management strategy. It intersects with claims integrity, credentialing, member experience, and regulatory readiness.
A mature approach integrates validation outputs into core systems rather than treating directory updates as isolated tasks. That integration enables audit defensibility and reduces manual reconciliation.
For a comprehensive view of how directory accuracy fits within enterprise provider data management, refer to the full guide here.
Conclusion
Provider data accuracy is now a measurable compliance and operational mandate. Ghost providers, directory errors, and fragmented systems create audit exposure and member friction.
Reactive cleanup projects cannot sustain regulatory alignment. Continuous validation, structured scoring, and system integration define the next stage of provider directory management.
Get in touch to explore how accurate provider data improves network performance →
