Provider data supports core payer workflows, from provider onboarding and directory management to claims processing and network operations. For health plans, maintaining accurate provider information is an operational requirement, not just a data quality burden.
At the center of these processes is provider roster management—the process through which provider groups submit updates about healthcare providers and their locations, specialties, and affiliations to health plans. Provider rosters help ensure that provider databases, claims systems, and member-facing directories remain accurate and up to date.
As provider networks expand and delegated relationships grow, healthcare roster management has become increasingly complex. Health plans now receive thousands of roster updates from provider groups across multiple markets, often in inconsistent formats that require extensive manual review.
Organizations are therefore turning to automation and AI-driven technologies to modernize roster management in healthcare. These approaches reduce manual data transformation, apply configurable business rules consistently, and move validated provider updates into downstream systems faster.
In this guide, we explore how healthcare roster management works, the challenges organizations face today, and how modern provider roster automation enables faster and more reliable provider data workflows.
What Is Provider Roster Management?
Provider roster management refers to the process of receiving, validating, standardizing, and updating provider information submitted by provider groups or delegated entities.
Provider rosters typically contain hundreds of data attributes such as provider identifiers, specialties, practice locations, affiliations, and network participation details. These submissions ensure that the health plan’s provider database reflects the most current provider information.
Once received, roster files must be validated and reconciled against existing provider records before updates are applied across internal systems. This process ensures provider data remains consistent across provider databases, claims systems, and member-facing directories.
Effective healthcare roster management helps accelerate provider onboarding, maintain more accurate provider directories, and reduce downstream issues tied to incorrect provider data. For organizations managing large provider networks, even small inefficiencies in roster workflows can create operational delays across multiple downstream systems.
Why Accurate Provider Rosters Matter
Certain core payer operations rely on accurate provider roster data, making healthcare roster management a critical function for health plans. Provider data impacts everything from onboarding new providers to maintaining compliant directories and ensuring claims are processed correctly. When roster data is inaccurate or delayed, the effects ripple across multiple systems.
One of the most immediate impacts is provider onboarding. When new providers join a network, their information must be validated and added to the provider database before they can begin seeing members under a health plan. Inefficient provider roster management workflows can delay this process, slowing network expansion and limiting access to care for members.
Provider rosters also play a significant role in provider directory accuracy. Federal and state regulations increasingly require health plans to maintain up-to-date directories so members can easily identify in-network providers. Meanwhile, inaccurate provider data continues to be a widespread challenge for health plans and provider organizations.
Accurate roster management also directly affects claims processing. Claims systems rely on provider records to verify network participation and determine reimbursement eligibility. When provider data is incorrect or outdated, claims may be denied or routed for manual review, creating additional administrative work for both providers and health plans.
Beyond operational workflows, reliable provider data ultimately improves the member experience. When directories are accurate and provider information is up to date, members can confidently identify available providers and avoid unexpected billing issues.
Common Challenges in Provider Roster Management
Despite its importance, roster management in healthcare remains highly manual for many organizations. Health plans often receive provider rosters from multiple provider groups and delegated entities, each using different formats and data structures. These inconsistencies make it difficult to process roster submissions efficiently and maintain accurate provider data across systems.
Non-Standard Roster Formats
Provider groups frequently submit roster files as spreadsheets or custom templates. Because these files rarely follow a consistent structure, operations teams must manually review and transform the data before it can be processed.
Industry initiatives have highlighted this issue for years. Organizations such as the Council for Affordable Quality Healthcare (CAQH) have emphasized the need for more standardized provider data exchange across healthcare organizations to improve data accuracy and reduce administrative burden.
High Attribute Volume and Reconciliation Complexity
Roster submissions often include many provider attributes, from identifiers and specialties to locations, affiliations, and participation details. Each submission must be checked against existing provider records before updates can be applied.
Manual Validation and Backlog Risk
When intake, standardization, validation, and reconciliation depend on manual effort, backlogs build quickly. That slows provider updates and increases the likelihood of downstream data issues.
Delegated Network Complexity
Delegated arrangements add another layer of operational difficulty. Health plans may receive roster submissions from multiple delegated entities, each with its own formatting conventions, timing expectations, and data quality issues. As those networks expand across markets, manual workflows become harder to scale consistently.
As provider networks expand, these challenges make traditional healthcare roster management workflows increasingly difficult to scale without automation.
Roster Management Across Health Plans, TPAs, and Delegated Entities
Provider roster management does not look the same across every type of organization. For health plans, the challenge is often scale: large provider networks, multiple markets, and high volumes of roster submissions that affect onboarding, directories, and claims operations.
For TPAs, the burden may be tied more to fragmented intake processes, limited operational capacity, or the need to coordinate provider data across multiple client environments.
In delegated models, roster management becomes more complex because provider groups or delegated entities may submit updates in different formats and on different timelines. That variability makes standardization, validation, and reconciliation more difficult without a more governed workflow.
Across all three environments, the underlying need is similar: process provider roster submissions accurately, apply the right rules consistently, and move validated updates into downstream systems without unnecessary delay.
Manual vs Automated Roster Management
For many healthcare organizations, roster management in healthcare has relied on manual workflows. Operations teams receive roster submissions, review them for formatting issues, map data fields to internal systems, validate records, and reconcile discrepancies before updates can be applied.
While these processes can work for smaller provider networks, they become difficult to scale as networks expand and submission volumes increase. Manual workflows require significant operational effort and often lead to delays in processing provider updates.
Provider roster automation helps modernize these workflows by reducing manual intervention across intake, standardization, validation, and reconciliation. Rather than relying on staff to transform each submission manually, automated workflows support more consistent processing across formats, provider groups, and markets.

By adopting provider roster automation, healthcare organizations can reduce processing times while improving provider data accuracy and operational efficiency.
How AI Enables Modern Provider Roster Management
AI supports specific workflow steps in modern provider roster management. This includes interpreting incoming roster files that follow different templates or naming conventions, allowing organizations to ingest roster submissions without requiring a single standardized format.
Once data is ingested, AI models can standardize provider attributes across hundreds of data fields. This ensures that provider records remain consistent across provider databases, claims systems, and provider directories.
AI also supports configurable rule-based validation, allowing organizations to create and apply complex business rules that reflect operational policies and regulatory requirements. These rules help identify missing data, incorrect codes, and inconsistencies before provider updates are applied.
Another key capability is data reconciliation. AI systems compare incoming roster submissions with existing provider records to identify updates and ensure that only validated data is applied across downstream systems.
Together, these capabilities allow healthcare organizations to scale provider roster management while maintaining high levels of data accuracy.
Key Capabilities and Best Practices for Scalable Provider Roster Management
A scalable provider roster management system must support both automation and operational governance. As provider networks expand across markets and delegated relationships grow, organizations need capabilities that not only process roster submissions efficiently, but also apply business rules consistently and connect reliably with downstream systems.
Core capabilities typically include:
- Multi‑format roster ingestion without requiring a single standardized template, allowing organizations to accept submissions from diverse provider groups while maintaining intake governance
- Standardization of incoming data into consistent provider attributes, ensuring provider records remain aligned across databases, directories, and claims systems
- Configurable business rules that can be applied by market, line of business, or provider group to reflect operational policies and regulatory requirements
- Validation and reconciliation against existing provider records, helping ensure updates are accurate before they flow downstream
- Visibility into exceptions, mismatches, and processing status, enabling operations teams to identify bottlenecks and reduce rework
- Integration with downstream systems such as provider databases, claims platforms, and directories, so roster workflows support end‑to‑end operations rather than operate in isolation
Together, these capabilities support best practices for modern roster management—standardizing intake even when source files vary, applying rules consistently, reconciling updates before activation, and monitoring operational performance over time.
By combining automation with governed workflows, healthcare organizations can scale provider roster processing while maintaining high levels of data accuracy and operational consistency.
How AI-Driven Roster Automation Works
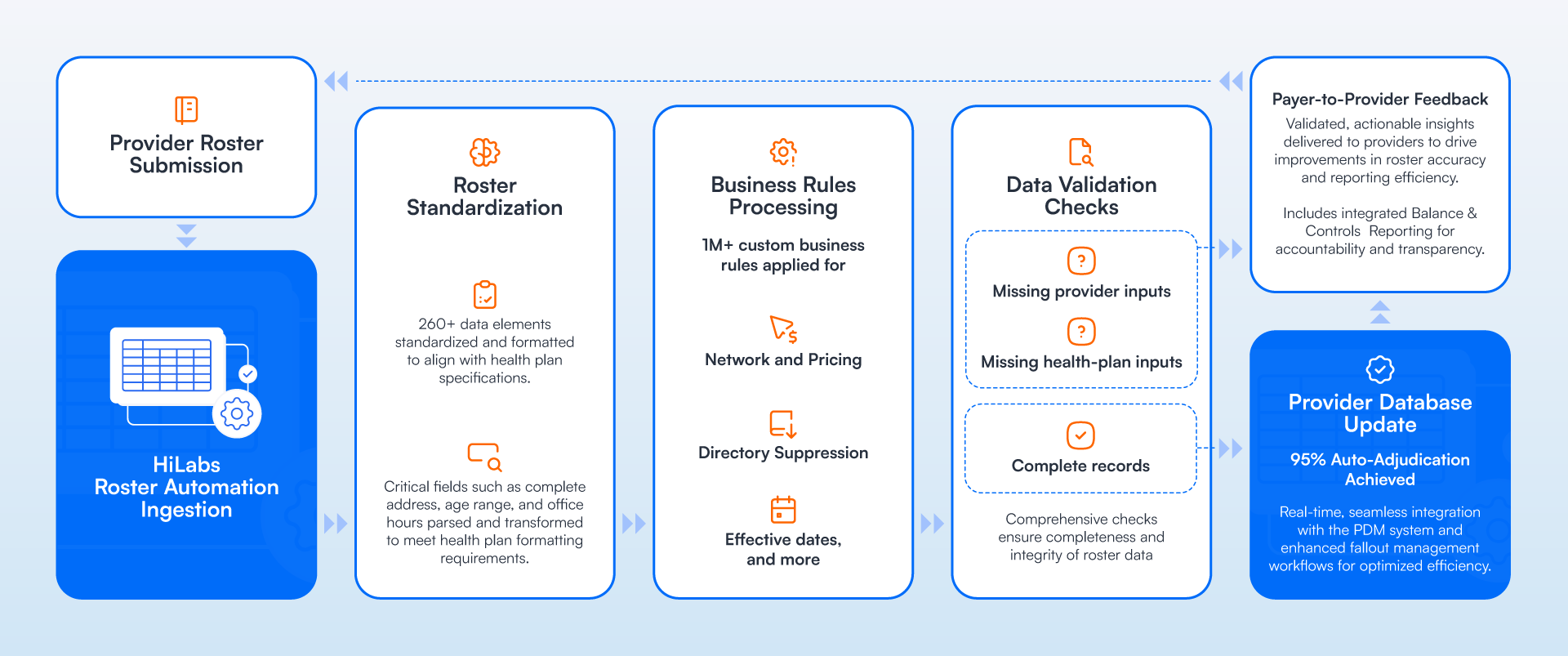
AI-driven roster automation platforms combine ingestion, validation, and reconciliation into a unified workflow.
When a roster submission is received, the system first ingests the file and interprets its structure. AI models map fields to standardized provider attributes used within the organization’s provider database.
Next, configurable business rules validate the submission by verifying provider identifiers, confirming code values, and identifying inconsistencies with existing provider records.
The system then reconciles incoming roster data with existing provider records to determine which updates should be applied. Once validation and reconciliation are complete, the updated provider information is distributed across downstream systems such as provider databases, claims platforms, and provider directories.
In more mature workflows, this process may also support integration with upstream intake processes and downstream operational systems, helping reduce manual handoffs across the broader provider data environment.
Solutions such as HiLabs® MCheck® Roster Automation use healthcare-specific AI to standardize and validate provider data across hundreds of attributes while applying configurable business rules that support data accuracy at scale.
Outcomes: Efficiency, Accuracy, and Provider Experience
Documented roster automation deployments have shown measurable improvements in turnaround time, processing efficiency, and provider data quality.
Processing times improve significantly as manual data transformation and validation steps are automated. Documented outcomes include reducing roster turnaround time from more than 21 days to less than 48 hours.
Automation also improves data accuracy by ensuring that validation rules are applied consistently across submissions. This reduces the likelihood of incorrect provider records entering the provider database.
Operational efficiency improves as organizations process larger volumes of roster submissions without expanding provider operations teams. By eliminating manual data transformation and reconciliation tasks, staff can focus on higher-value work.
Faster and more reliable roster processing improves the provider experience. Providers can be onboarded more quickly, directories remain accurate, and administrative friction across provider networks is reduced.
Conclusion
As provider networks continue to expand, managing provider data accurately and efficiently is becoming increasingly complex. Traditional approaches to provider roster management rely on manual workflows that create delays, introduce errors, and strain operational teams.
AI-driven automation is transforming this process by streamlining ingestion, validation, and reconciliation of provider rosters. By adopting scalable provider roster automation, health plans can maintain accurate provider directories, improve operational efficiency, and deliver a better experience for both providers and members.


