VBC Data Ingestion
All plan-specific inputs are captured and prepared for analysis.
Ingest VBC input data from multiple sources
Include member attribution, financial transactions, and payment models
Consolidate data for unified processing










Legacy processes rely on manual workflows, siloed systems, and delayed insights. MCheck VBC uses AI-driven automation to validate attribution, detect anomalies in real time, and improve payment accuracy at scale.
| Traditional Systems | VBC Caresphere |
|---|---|
| Manual attribution reviews limit coverage and scalability | Real-time attribution validation across all provider groups and programs |
| Incomplete analysis leads to missed anomalies | Identifies anomalies with complete coverage |
| Reactive processes delay issue identification and resolution | Provides root cause analysis (RCA) for faster, actionable insights |
Comprehensive, AI-powered solution designed to detect, resolve, and prevent value-based care payment issues at scale
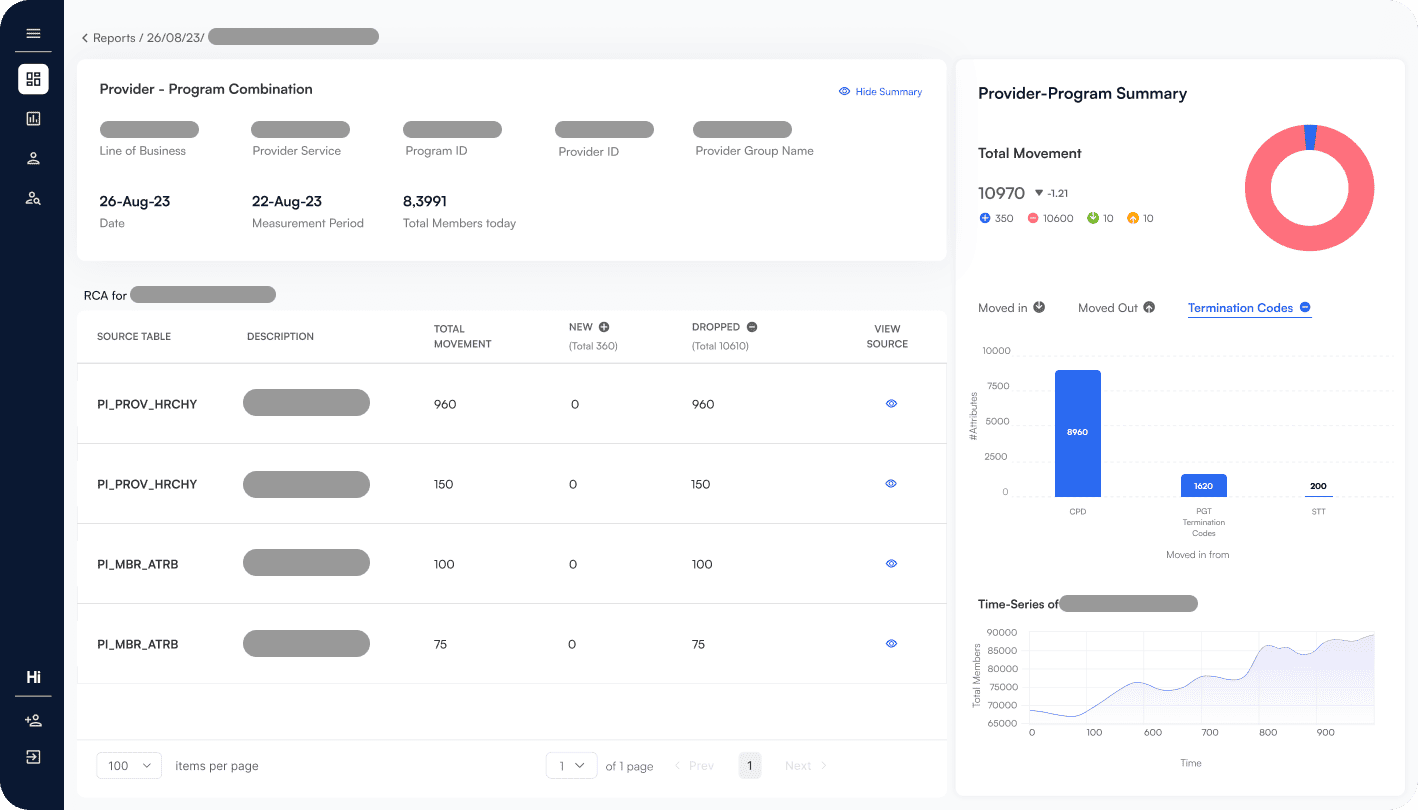
Anomalies identified across member attributions and provider payments
Provider groups analyzed daily for anomalous attributions
Financial transactions audited monthly for anomalous payments
MCheck VBC transforms fragmented inputs into validated insights, enabling real-time anomaly detection, root cause analysis, and accurate provider payouts across value based care programs.
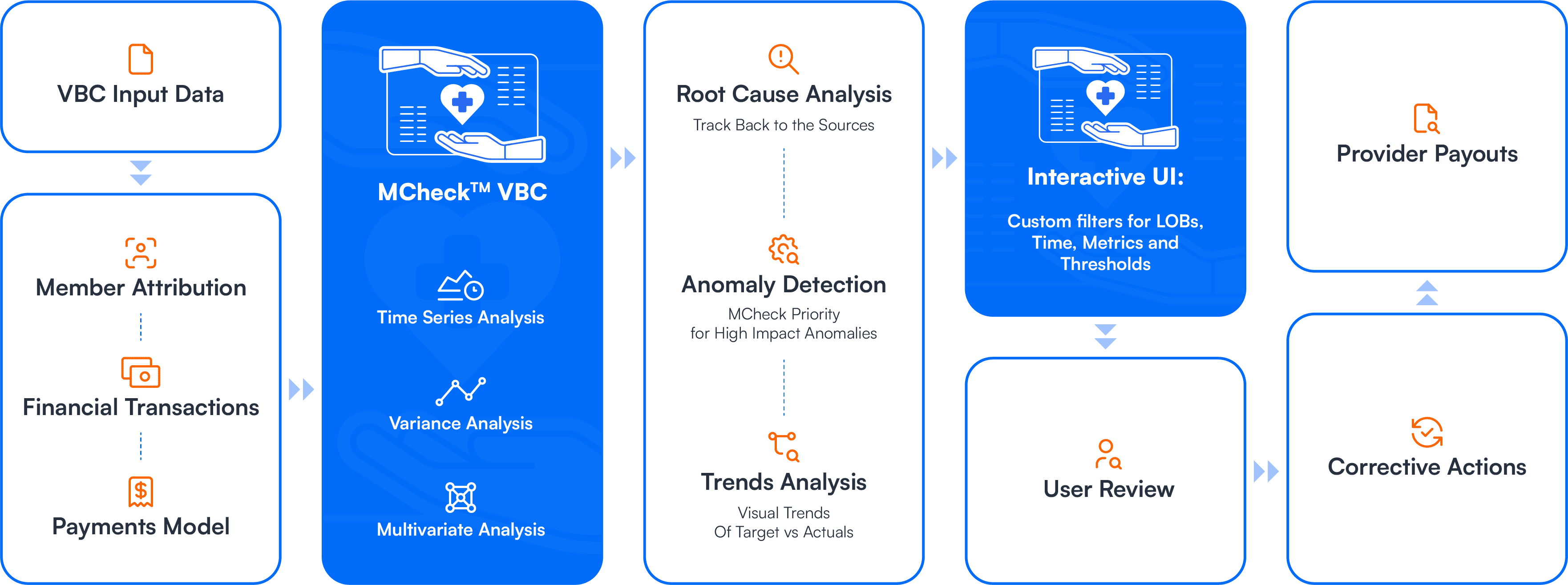
All plan-specific inputs are captured and prepared for analysis.
Ingest VBC input data from multiple sources
Include member attribution, financial transactions, and payment models
Consolidate data for unified processing
AI models analyze data across multiple dimensions to identify patterns.
Perform time series analysis to track changes over time
Run variance analysis to detect deviations
Apply multivariate analysis for deeper insights
The system identifies and prioritizes high-impact issues.
Detect anomalies across attribution and payments
Prioritize issues based on impact and severity
Surface critical discrepancies for action
Issues are traced back to their source with contextual insights.
Perform root cause analysis for detected anomalies
Analyze trends comparing target vs actuals
Provide actionable insights for resolution
Users interact with insights through a flexible interface.
Use custom filters by LOBs, time, metrics, and thresholds
Enable user review and validation of findings
Support faster, data-driven decisions
Insights drive actions that improve payment accuracy.
Trigger corrective actions for identified issues
Ensure accurate provider payouts
Continuously improve VBC program performance
See how leading health plans improve attribution accuracy, reduce payment leakage, and drive measurable cost savings across value based care programs with AI-powered automation.

HiLabs AI-driven anomaly detection and root cause analysis have significantly reduced manual effort, streamlined workflows and unlocked millions in cost savings
Accurate payments and real-time member attribution have driven transparency and trust, leading to meanignful reductions in provider disputes
With clearer insights and targeted engagement, provider participation in VBC programs has increased significantly across supported markets

Purpose-built platforms that bring accuracy, intelligence, and automation across provider data, networks, contracts, value-based care, and clinical operations.